
Breast Health Awareness
When talking about breast health, most women think of cancer as their primary concern. While breast cancer is a serious health problem, many breast conditions are not necessarily associated with breast cancer. These conditions often do not indicate breast cancer, though it is best to discuss them with your healthcare practitioner.
Women commonly seek medical attention because they have found a lump or are experiencing pain in their breasts. Finding a lump may be frightening, even when it is diagnosed as benign. Understanding the anatomy of your breasts–including how they function and what types of disorders may occur—is the first step in minimizing that feeling of vulnerability.
Breast Anatomy
 Breasts come in all shapes, sizes, and textures; some are lumpy, some are smooth, some are firm, and some sag. Most women have one breast that is slightly smaller than the other, and some women’s breasts may change from month to month.
Breasts come in all shapes, sizes, and textures; some are lumpy, some are smooth, some are firm, and some sag. Most women have one breast that is slightly smaller than the other, and some women’s breasts may change from month to month.
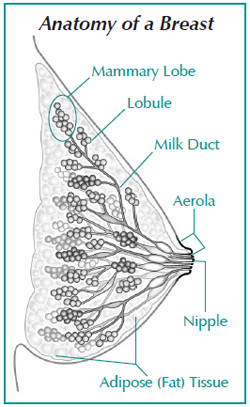
Breasts contain multiple lobes, which are divided into smaller lobules that contain glands for producing milk. The area between the lobes is cushioned with fat and fibrous tissue that attaches the breast to the chest muscles. Breast tissue extends up into the armpit or axillary area, which also contains lymph nodes that help eliminate bacteria, dead cells, and other harmful substances. Breasts also contain extremely sensitive nerves, which account for their sexual response, connecting them with the female genital system.
Breast tissue is not typically homogeneous; one area may feel denser during examination than another area simply because it contains more fibrous connective tissue than soft fat. It is also common for the connective tissue-to-fat ratio to change as a woman ages.
In Women’s Bodies, Women’s Wisdom, Dr. Christiane Northrup explains that female breasts are glandular organs loaded with hormone receptors. This makes breasts sensitive to even small hormonal changes in the body. Breasts go through cyclical changes that coincide with the menstrual cycle, pregnancy, and childbirth.
Hormonal Fluctuations
Each month, the breasts prepare for the possibility of pregnancy in response to the ebb and flow of female hormones (primarily estrogen, progesterone, and prolactin). During the first half of the menstrual cycle, the ovaries produce estrogen hormones in increasing quantities, stimulating cell growth in the glands, ducts, and fibrous tissues of the breasts. This increase in cell activity leads to increased blood flow to the breast, which some women experience as fullness or tenderness.
In the middle of the menstrual cycle, the ovary releases an egg, stimulating the release of progesterone into the bloodstream. Progesterone provides additional stimulation to the gland cells, further increasing the blood flow and amount of fluid seeping from the ducts into the breast tissue, which makes some women’s breasts feel heavy or painful, three to four days before their period. During pregnancy, the body produces prolactin, which triggers the production of breast milk at delivery.
If pregnancy doesn’t occur, hormone levels shift again as menstruation begins. The changes in the breast that the hormones stimulated are reversed. The swelling of breast tissue diminishes and the breast softens.
In a healthy breast, new cell growth and fluid production subside and the thickening, lumps, and pain usually disappear fairly quickly. Lumps that persist or reoccur might indicate a breast condition. The best course of action is to report any breast lump, pain, or concern you have to your healthcare practitioner.
Breast Cancer
The specific causes and cures for breast cancer are as yet unknown. For many years, cancer treatments have been based on the idea that cancer develops due to rampant cell growth. While that is partly true, scientists have discovered that it is more likely that growth results from the failure of a self-destruct mechanism in bad cells.
The body’s cells are constantly being compromised or damaged by carcinogens, free radicals, and other harmful substances. Normally, the damaged cells are quickly eliminated through a pre-programmed process of cell death, called apoptosis. If apoptosis fails, however, the cancerous cells continue to divide and grow unchecked, resulting in tumors.
Estrogen and Breast Tissue
Breast tissue is highly sensitive to hormones, especially estrogen. The presence of estrogen encourages breast cells to multiply. (This helps explain why men develop breast cancer less often, even though they also have breast tissue: they have less exposure to estrogen than women.)
Estrogen is associated with most breast cancer cases. Two distinct types of breast cancer have been identified: a more common estrogen-dependent form, and a less common non-estrogen-dependent form. Many medical professionals and researchers believe that the prevalence of breast cancer is due to prolonged exposure to estrogens, particularly “foreign” estrogens (that is, estrogens not produced by the body).
Modern medicine has expanded women’s “estrogen window,” with earlier exposure to estrogen via oral contraceptives, followed by estrogen replacement therapy later in life. Increased exposure to estrogen increases the risk of developing breast cancer. This is particularly true when progesterone has not been prescribed as part of a balanced hormone replacement therapy.
Breast Cancer Risk Factors
Lifestyle Choices
- Early or excessive use of tobacco
- Bras and other clothing, worn tight enough to restrict the lymph system
Modern Medicine
- Some non-hormonal prescription drugs, such as anti-hypertensives
- Silicone gel breast implants, especially those covered with polyurethane foam
Environmental Factors
- Exposure to chemicals, pollutants, and carcinogens, such as those found in household cleaners, paints, etc.
- Proximity to chemical plants or hazardous waste sites
Personal/Family History
- Previous incidence of breast cancer
- Diagnosis of fibroids on a breast biopsy
- Early menstruation (before age 12) and/or late menopause (after age 50)
- Close relatives (i.e., mother, sister, aunt, or grandmother) with breast cancer
- Certain ethnicities (e.g., European Jews and Northern Europeans)
Unchecked by progesterone, estrogen may lead to uncontrolled growth of breast tissue, including cancer. Progesterone is necessary to limit the growth and direct it into a different type of cell, which eventually dies off naturally. According to Dr. Northrup, evidence suggests that progesterone may reduce not only the spread of breast cancer but also the incidence of new cases.
Reproduction’s Influence on the Breast
Reproductive circumstances affect a woman’s risk of breast cancer. Not having children, or having them at a later age, thwarts or delays the maturation of breast tissue. Breast cells reach complete development only when a woman goes through a full-term pregnancy; until then, the immature breast cells are more susceptible to abnormalities, which may be stimulated by estrogen and/or triggered by carcinogens and other toxic substances. This is one of the primary reasons that early or prolonged exposure to any harmful or toxic substance is a higher risk for young females and any woman without fully developed breast tissue.
Other Breast Disorders
Some healthcare practitioners place breast lumps and pain in the catchall category of “fibrocystic breast disease.” Many women who are told that they have this condition are simply experiencing normal changes in breast anatomy. The three most common breast disorders are more accurately described as fibrosis, cysts, and problems with the milk ducts.
Fibrosis is the thickening of the breast’s connective tissue, which itself is not typically painful. However, fibrosis is often accompanied by the formation of cysts because the tissue growth blocks the milk ducts, causing them to swell into tender, fluid-filled sacs, which may feel like lumps. Other pains and lumps usually result from hormonal changes, which may be aggravated by diet, stress, or other lifestyle factors.
Fibrocystic breast disease (also sometimes called cystic mastitis) is believed to be associated with an elevated estrogen-to-progesterone ratio. This disease may also be related to iodine levels in the body. Both Dr. David Derry’s Breast Cancer and Iodine and Dr. David Brownstein’s Iodine: Why You Need It, Why You Can’t Live Without It observe that iodine supplements have been effective in treating fibrocystic breast disease.
Breast Tenderness or Pain
Breast pain, sometimes called cystic mastalgia, typically comes and goes with the menstrual cycle. It is usually caused by an increase in hormonal stimulation of the breast from an excess of the estrogen hormones, an excess of caffeine, or chronic stress. In some women, breast pain may be premenstrually severe or become a month-long problem.
According to Dr. Robinson Baker, chronic or severe breast pain is often related to hormone imbalance (usually either too much estrogen or too little progesterone). It may also be influenced by other body chemicals resulting from stress or stimulated by certain foods, as well as other hormones. Dr. Baker advises testing hormone levels if chronic breast pain continues even after making dietary changes.
Lumps or Cysts
What women sometimes perceive as lumps is often simply thick connective tissue or fluid-filled glands. Occasionally, one of these glands may swell and feel hard. Women with a more generous supply of fat or denser connective tissue are more likely to mistake normal breast anatomy as something to be concerned about.
Lumps from small cysts often diminish over time. For younger women, a healthcare practitioner might suggest watching it for several menstrual cycles to see if it goes away. Larger lumps may be aspirated (drained with a needle) or surgically removed.
Cysts are usually not cancerous, with eight out of ten being benign. In Natural Hormone Balance for Women, Dr. Uzzi Reiss says that “there is no connection between the common lumps and breast cancer, as long as a woman is not in estrogen dominance.” He promotes a progesterone supplement to balance the excess estrogen.
Nipple Discharge
Nipple discharge may be alarming but is not dangerous. After nursing a baby, it may take a year or more for the milk-producing glands to stop completely. Some women experience a nipple discharge (a liquid that may vary from a greenish clear to a pale milky substance) during the stimulation of sexual contact. However, bloody discharge is not normal and should be reported to your practitioner immediately.
Monitoring Breast Health
Mammograms (X-rays of a compressed breast) are endorsed by most cancer organizations and many healthcare practitioners for any woman over age 50 and are encouraged for women over the age of 40 if there is a history of breast cancer or other breast disorders. Mammography typically yields fairly reliable results with postmenopausal women, primarily because their breast tissue is less dense.
Mammography does not prevent breast cancer; it is simply a way to detect potential abnormalities. Mammography has come under scrutiny among some medical professionals for several reasons:
- Mammography may give women a false sense of security because it may miss detecting breast cancer.
- Mammograms do not show tumors that are “out of the picture” such as those in the armpit or near the collar bone where the lymph nodes are located. They are also not suitable for women with particularly dense breasts because visibility of growths may be reduced.
- The density of the breast in premenopausal women makes detection difficult, sometimes leading to either a false-negative or false-positive reading. The radiation itself is another potential hazard, especially for premenopausal women. Many studies have demonstrated a strong link between radiation and breast cancer.
- Because of the density of the breast tissue, many premenopausal women have to undergo several exposures to get a good reading. Some medical professionals believe that the total radiation dosage to which women are exposed is excessive.
Other factors to consider include the fact that higher levels of estrogen may make breast tissue more susceptible to the carcinogenic effects of radiation and, in rare cases, severe compression of breast tissue may cause an existing tumor to rupture. Talk with your healthcare practitioner about whether or not a mammogram is necessary or the best way to identify potential abnormalities.
Other Diagnostic Methods
Thermograms do not require radiation, contact, or breast compression. They work by detecting tiny variations in blood vessel activity and displaying an infrared image. This is used to target potential precancerous sites or the presence of an early tumor that is not yet large enough to be detected by mammography.
No matter how a lump or suspicious area is detected, your healthcare practitioner will likely pursue a diagnosis to ensure that it is not breast cancer. They might request a non-invasive procedure, such as an ultrasound, diagnostic mammogram, or magnetic resonance imaging (MRI) to further differentiate the growth. A definitive diagnosis usually requires aspiration and biopsy of the tissue cells.
Lifestyle Choices
Effects of Diet on Breast Health
Assuming breast lumps or pain are not due to cancer (as is the case most of the time), there are several things you can do to reduce pain or tenderness in your breasts or nipples:
Research indicates that eliminating foods containing caffeine reduces breast pain and cysts in most women within a few months.
Reduce alcohol consumption. Alcohol boosts estrogen levels, which might have minor beneficial effects for some postmenopausal women not on ERT. However, women on ERT face additional risks from consuming even small amounts of alcohol. Just a half glass of wine may increase the circulating estrogen to an unacceptable level, thereby increasing breast cancer risk.
Eat a healthy diet. Many in the United States eat a diet high in calories and animal fat. Many foods are contaminated with pesticides, fertilizers, and “foreign” hormones such as those found in some meat or dairy products.
Food contaminants tend to accumulate and concentrate in body fat, particularly in the abdominal area and breasts. Similarly, avoid trans fats found in many processed foods, as they introduce free radicals into our bodies, potentially leading to cell damage.
Breast problems are associated with a low-fiber diet and chronic constipation. Women with severe constipation (i.e., less than three bowel movements per week) are more likely to show signs of possible abnormal cell production. This may be because estrogen secreted by the liver is more readily reabsorbed by women with slow digestion.
Foods recommended for healthy breasts include fresh or dried fruits, vegetables, whole grains, beans and legumes, and some fish. Drinking 8-10 glasses of water per day will help detoxify the body. Some healthcare practitioners recommend supplements of vitamins E, A, and B to reduce breast pain and lumps.
Stress and Exercise
Fibrocystic breasts may be more responsive to changes caused by adrenaline, which is produced during stressful situations. Reducing stress by exercising seems to have a positive effect on reducing or eliminating breast problems.
While alleviating stress, exercising also reduces body fat, including fat cells in the breast. Because estrogen is stored in fat cells, women with a high percentage of body fat may experience enhanced estrogen production, causing breast tenderness. Women who consistently exercise tend to have fewer breast problems and a lower rate of breast cancer.
Conclusion
Maintaining breast health requires regular monitoring of your breasts so that you can quickly identify anything unusual. The more risk factors you can eliminate or avoid, the better your chances of decreased breast cancer risk. Becoming informed and proactive in your defense against breast cancer and other diseases extends to small, daily choices.
Connections is a publication of Women’s International Pharmacy, which is dedicated to the education and management of PMS, menopause, infertility, postpartum depression, and other hormone-related conditions and therapies.
This publication is distributed with the understanding that it does not constitute medical advice for individual problems. Although this material is intended to be accurate, proper medical advice should be sought from a competent healthcare professional.
Publisher: Constance Kindschi Hegerfeld, Executive VP – Women’s International Pharmacy
Co-Editors: Michelle Violi, PharmD; Laura Strommen – Women’s International Pharmacy
Writer: Carol Petersen, RPh, CNP – Women’s International Pharmacy
Illustrator: Amelia Janes – Midwest Educational Graphics
Copyright © Women’s International Pharmacy. This newsletter may be printed and photocopied for educational purposes, provided that your copy (or copies) include full copyright and contact information.
 For more information, please visit womensinternational.com or call 800.279.5708.
For more information, please visit womensinternational.com or call 800.279.5708.
Women’s International Pharmacy | Madison, WI 53718 | Youngtown, AZ 85363

