
Probiotic Potential
Using “Friendly” Bacteria to Promote Healthy Digestion, Strengthen Immunity, and More
A probiotic—literally, “for life” in Greek—is defined as “a preparation or a product containing a sufficient number of live microorganisms to alter the flora of the host and bring about beneficial health effects.” In short, probiotics are “friendly” bacteria (and sometimes fungi) that we import into our system to hold more dangerous microbes in check. A growing number of scientific studies have found that probiotics may aid both digestive and immune system health.
Yogurt, aged cheese, and many other cultured and fermented foods make up this category of “superfoods.” Yogurt, the most popular probiotic, has been around at least 4,000 years and for centuries has been linked to long life. In the early 1900s, the Russian immunologist Ilya Mechnikov received a Nobel Prize for his studies on the unusual longevity of Bulgarian peasants. He learned these peasants ate a diet high in fermented foods, including yogurt and other foods containing a bacterium he named Lactobacillus bulgaricus.
Probiotic foods or supplements are generally safe and widely available. Most people find them both tasty and easy to digest. But are they effective? Is it a “one size fits all” solution, or should some people seek particular types of probiotics? How can you make sure you’re getting enough probiotics to make a difference? To take full advantage of probiotics, you need to begin by learning about the place you want them to wind up: the human microbiome.
The Human Microbiome: Welcome Inside “Microbe City”
The microbiome organ is a collection of microbes or single-celled microorganisms—called microflora—that live on and in the body. The human body contains 100 trillion cells, and 90% of them are not even our own—nearly all of these are bacteria; the rest are yeasts and parasites. These microbes are incredibly diverse in size, shape, color and growth rates, and may include as many as 1,000 different species.
The microbiome begins developing at birth and changes throughout our lifetime. The environment plays a larger role in determining microbiome makeup and health than genetics, which explains why members of the same household may have similar conditions even without being genetically related.
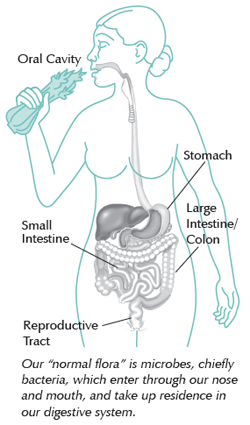
Microbes enter our body through the air we breathe, and the food and drink we consume. Once stuck in the mucus that lines our oral and nasal cavities, they are swallowed and propelled through our digestive system. Most of these bacteria, called “normal flora,” reside in the GI tract, primarily in the places shown in the figure to the right, including:
- Oral Cavity (the mouth, nose, and throat): Millions of bacteria live in a single teaspoon of saliva, including “bad” types linked to halitosis and gingivitis.
- Stomach: Few bacteria live here due to high acidity, but one is Heliobacter Pylori, which can cause ulcers and stomach cancer. Lactobacillus may help keep Pylori in check.
- Reproductive Tract: A healthy vagina contains thousands of different types of bacteria, with the majority being a type of Lactobacillus.
- Small Intestine: Millions of bacteria live in this organ, where they receive nutrients in exchange for helping digest food, make vitamins, and stimulate the immune system. Most of these bacteria are benign species of Streptococcus and Enterococcus.
- Large Intestine (Colon): Billions of bacteria, predominantly Bacteroides, live in the colon or large intestine, the final step in digestion where wastes are stored and excreted in the stool. Stool contains over 500 different types of bacteria.
In this teeming “inner city” of the microbiome, microbes compete for food and space in the mucosal surfaces lining the digestive tract. The relationship is symbiotic: the human body gives the microbes room and board in exchange for labor, mainly breaking down food.
Although there are widespread “employment opportunities” for microbes in food digestion, most digestive organs offer lousy accommodations. The acid and churning causes many microbes to migrate to the intestines with their long coils of mucosal folds. Most gut bacteria reside in the colon, where water is absorbed from indigestible food matter and waste is stored before being removed from the body.
Among our body’s microbes, you can find the “good” (probiotics like Lactobacillus, a common bacteria in yogurt), the “bad” (bacteria that usually result in serious illness, such as Salmonella), and the “risky.” In this final group are several bacterial species that are beneficial when they are in the right place and quantity, but may lead to health issues if their numbers are unbalanced or if they are located in the wrong part of the body. For example, species of Klebsiella make vitamins B12 and K when they’re in the small intestine, but may cause pneumonia when they’re inside the lungs.
In a healthy gut, friendly bacteria are plentiful enough to keep dangerous and potentially harmful bacteria under control. Unfortunately, Gary B. Huffnagle, PhD, a professor of internal medicine, microbiology and immunology at the University of Michigan Medical Center, notes that most people are lacking in friendly bacteria.
Aside from their role in proper digestion, Dr. Huffnagle maintains that microbes are also vital to our immune system. As he writes in The Probiotics Revolution, microbes “send signals to the immune system that reduce destructive overreactions, including inflammation. This means that insufficiencies affect immune responses—and therefore every aspect of our health.” (The chart below identifies some of the autoimmune disorders suspected to be associated with specific bacteria.)
The Microbiome’s Effect on Hormones
In addition to affecting our immune system, the microbial imbalance in our gut can affect other systems in our body, including our hormonal system. The digestive system plays an important role in the proper disposal of estrogens from the body. When the flora in the intestines is disturbed, estrogen that should be excreted may instead be recycled into the bloodstream, creating hormone imbalance.
The development and changing of the microbiome over time may coincide with other physical changes. Many major life changes such as puberty, pregnancy, and menopause that affect the microbiome also affect hormone balance: University of Utah’s webpage Your Changing Microbiome provides just a few examples, saying: “puberty affects skin microbes by causing changes in skin oils. And pregnancy brings on changes in the vaginal microbiome: species start to grow that will colonize and benefit the baby as it’s born.”
Suspected Associations Between
|
|
| Disorder | Type of Bacteria |
| Ankylosing Spondylitis | Klebsiella |
| Graves’ disease and Hashimoto’s disease | Yersinia |
| Guillain-Barre syndrome | Campylobacter |
| Multiple sclerosis | Chlamydia |
| Rheumatic fever | Streptococcus Pyogenes |
| Rheumatoid Arthritis | Citrobacter, Kiebsiells, Proteus, Porphyromones |
| Autoimmunity, in general | Escherichia coli, Proteus |
The Gut as an Immune Organ
According to Kelly Dowhower Karpa, PhD, RPh, the GI tract is the largest immune organ in the body. In her book Bacteria for Breakfast, Dr. Karpa describes how gut bacteria communicate with immune system cells within the walls of our intestines. This instant messaging helps ensure immune cells fight disease-causing substances while tolerating normal foods and flora; as we grow up, this “oral tolerance” becomes the foundation of a mature immune system.
“Normal gut bacteria acquired in infancy are likely to be the most important determinants of allergies and diseases of chronic inflammation later in life,” Dr. Karpa writes. Some studies show taking probiotics during pregnancy may help prevent babies from developing eczema, notes Dr. Huffnagle, who adds that probiotics are “under intense investigation as an allergy treatment.” He believes that probiotics may also be used to help autoimmune diseases “because they signal the immune system to show restraint.”
Allergies
Allergic reactions happen when the immune system overreacts to harmless substances. Dr. Karpa says that the incidence of immune-related conditions, from allergies to inflammatory diseases, has increased in Western societies since the late 1950s. Many researchers believe environmental changes are involved: in particular, increased hygiene practices and unbalanced, processed-food diets.
To Dr. Karpa, this indicates that “exposure to various types of bacteria—through dietary sources and by actually getting sick and letting the immune system do its job—makes a dramatic impact on the development of allergic diseases.” According to Dr. Karpa, the presence of bacteria in the gut stimulates cytokine production, which signals the immune system to trigger inflammation and allergies. Different species of bacteria stimulate the release of different cytokines.
The widespread use of antibiotics over the same period must also be considered, stresses S.K. Dash, PhD, founder and president of the probiotic company UAS Laboratories. “Antibiotics can be the biggest culprits in destroying our friendly bacteria,” Dr. Dash writes in The Consumer’s Guide to Probiotics. “At high dosages, they can wipe out all bacteria inside your body, the good along with the bad. Once that happens, the race is on to as to which microorganisms, the good guys or the bad guys, set up shop.”
Even without taking antibiotic medications, Dash points out that meat-eaters still consume them, since most US cattle, pigs and poultry receive antibiotic feed. He urges those taking prescription antibiotics to use probiotics at the same time to replenish friendly microbes.
Inflammatory Bowel Disease, Crohn’s Disease, and Irritable Bowel Syndrome
Immune system malfunction sometimes leads to chronic inflammation of the intestines, resulting in inflammatory bowel disease (IBD), which affects 60-70 million Americans. Specific forms of this disease range from the relatively mild Irritable Bowel Syndrome (IBS) to a more severe form, Crohn’s Disease. Studies show that people with IBD have a greater tendency for microbial imbalance in the gut when compared with healthy people.
IBS is characterized by bowel pain, bloating, diarrhea or constipation, and gas. IBS has no known cause and doesn’t coincide with any visible damage to digestive organs, so it is diagnosed only after other forms of IBD have been ruled out. It affects three times as many women as men: as many as 20% of women in the US are believed to suffer from IBS at some point in their lives. Probiotics have had mixed results in treating IBS. However, one Irish clinical study showed significant improvement when IBS patients took a daily drink of Bifidobacterium infantis.
In Crohn’s Disease, deep inflammatory lesions affect the lower part of the small intestine and the colon. (A similar condition, ulcerative colitis, is characterized by smaller lesions plaguing only the colon.) The resulting thickening and swelling of the bowel wall can cause deep intestinal obstruction, which can become life threatening. Patients frequently endure cycles of extreme pain and weight loss with periods of remission.
Even when the immune system is not implicated, several common gastrointestinal illnesses—ranging in severity from mild stomach upset to life-threatening, chronic ailments—occur when there is an imbalance in the microbiome. Treatments include anti-inflammatory medications injected into the intestinal tract, immune-suppressive, and immune-modulatory medications. For some, however, medications fail and surgery is required.
Diarrhea
Diarrhea is often the result of viral gastroenteritis (usually caused by rotavirus or norovirus) or Traveler’s diarrhea (following ingestion of water contaminated by fecal bacteria such as E. coli). Some people develop severe diarrhea after exposure to an antibiotic-resistant strain of bacteria known as C. difficile. This often occurs in a hospital or other institutional setting, following a course of antibiotics.
Whatever its cause, acute diarrhea remains the world’s leading cause of illness and death. Dehydration may prove deadly where treatment is unavailable. Even with modern medical care, those who suffer from C. difficile often endure painful, recurring bouts with diarrhea whose symptoms may include a life-threatening form of colitis.
Probiotics are generally advised for preventing but not treating disease. In the case of diarrhea, however, some studies show probiotics may have healing properties: “Lactobacillus CG at high doses for 7-10 days after antibiotics has cured patients with relapsing C. difficile,” says Dr. Karpa. In addition, studies show Lactobacilli can treat and prevent rotaviral diarrhea, shortening the duration of diarrhea and speeding the healing process.
Candidiasis
A strain of yeast called Candida albicans (Candida for short) is a normal component of our digestive system. However, when pH becomes unbalanced—often by antibiotics or a diet high in sugar and starches—Candida overgrowth may occur, resulting in candidiasis (commonly called a yeast infection). This may cause a wide range of chronic digestive problems, such as bloating and heartburn.
Sometimes the Candida organism bores into the gut wall, releasing powerful toxins and incompletely-digested dietary proteins into the bloodstream. The immune system then produces antibodies, causing allergic reactions that may trigger a host of problems, including chronic fatigue, headache, and depression, as well as a multitude of food allergies. Bacteria in the gut inhibit the growth of yeasts by producing pH-lowering lactic acid (and sometimes other acidic substances).
Vaginal and Urinary Tract Infections
Candida overgrowth also occurs in other parts of the body, notably the vagina. Use of some medications, especially antibiotics, increases a woman’s risk for vaginal candidiasis. Symptoms are often treated by prescribing antifungal medications but typically recur unless the GI and genital tracts are replenished with friendly bacteria.
Probiotics have been shown to help restore the normal yeast-bacteria balance in the body. “Products that stimulate L. acidophilus or B. bifidum can help immensely as part of a comprehensive program that addresses the whole person,” says Dr. Dash.
Other imbalances in the vagina and the urinary tract may benefit from increased use of probiotics. For example, problems associated with vaginal inflammation (vaginitis) may affect women of all ages, causing vaginal discharge and pain. In younger women, these symptoms usually result from an imbalance of harmful bacteria. This may be serious when it occurs in pregnant women since it may cause premature labor.
Postmenopausal women often develop atrophic vaginitis—inflammation resulting when estrogen levels drop and the tissues become thinner and drier. This scenario increases vaginal pH and predisposes these women to vaginal pain and discharge and also to urinary tract infections (UTIs) and vaginal infections. Usually these infections are easily treated; however, they often recur. Additionally, the antimicrobials used to treat these infections further disrupt the microbial balance in the area.
Clinical evidence shows that probiotics may help prevent and even treat urogenital tract problems. In their chapter on these conditions in The Power of Probiotics, Dr. Gary Elmer et al. cite a clinical study of women who took freeze-dried L. rhamnosus GR-1 and L. fermentum RC-14. The results showed these women were less likely to get bacterial vaginosis, and that their levels of protective Lactobacilli bacteria were also higher, indicating protection from yeast overgrowth.
The Value of Probiotics
In general, probiotics promote healthy digestion. Microbes in the intestines make short-chain fatty acids (needed for GI tract health), antioxidants, amino acids, and vitamin K. Nutrients in fermented foods absorb more readily than nutrients in unfermented foods. Fermented foods use agents such as yeast, bacterium, molds, or enzymes to break down a substance into simpler substances; examples include converting milk to yogurt or cheese, fermenting soy to make miso, and fermenting cabbage to make kimchi or sauerkraut.
With growing alarm over the spread of virulent strains of antibiotic-resistant bacteria, many people are eager to try approaches to illness prevention and treatment that do not require the use of antibiotics. Getting a beneficial effect for individual health needs, however, depends on various factors, including:
- The strain of probiotics selected and how the body can use it
- The numbers of live probiotics in the purchased product, and whether they are stored and taken properly
In his book, Dr. Huffnagle remarks on the foresight of Chinese doctors centuries ago: “They somehow knew that the intestines were not merely a digestive organ, but the center of health and well-being.” Modern medicine is confirming their wisdom with clinical studies and laboratory tests, which add knowledge about the effects of various bacterial strains.
Safety, Storage, and Use of Probiotics
Probiotics are safe for the majority of people, except for those at high risk for infections of all types (such as those with HIV/AIDS or cancer), or those taking immune-suppressive steroids. It is always advisable to check with your practitioner before taking any new supplements, as probiotics do have the potential to interact with some medications. Moreover, your practitioner can help you select the probiotic that is best suited to treating your particular condition, notes Dr. Karpa: “You may have to search for the right probiotic, the appropriate number of microorganisms, or the necessary combination of probiotics until you find the right mix to successfully fill the bacterial niche missing in your gastrointestinal tract.”
Whether taken by pill (as a supplement) or by plate (in food), either form of probiotics can be effective as long as proper procedures of storage and ingestion are followed. Although it might seem that pill supplements would be required for the lactose-intolerant, that is not necessarily the case. Probiotics have been shown to help break down lactose, reducing symptoms of the illness and allowing sufferers to reintroduce dairy into their diet—at least in the form of yogurt and other fermented products.
Any form of probiotic should be purchased with care to ensure you are receiving the promised strain and quantity of live bacteria (or, in some cases, fungi), and that it has been properly stored. Foods containing live cultures must be kept refrigerated, and storage dates must be strictly followed. All too often, Dr. Karpa notes, the bacterial strains listed on a label are not the actual strains in the product.
In Acidophilus and Your Health, author Frank Murray includes this advice when purchasing yogurts:
- Always purchase yogurt with “live, active cultures,” including Lactobacillus acidophilus
- Avoid frozen yogurt or pudding-style yogurts, which have stabilizing chemicals and artificial sweeteners added
The possibility of inaccurate or misleading labels leads some to suggest cutting out the middleman; for instance, Murray also provides a recipe for making homemade yogurt.
Probiotic foods may not supply enough active bacteria or fungi to alter the microbiome (unless carefully made or purchased). To give probiotics a better chance of success, make sure to take them on an empty stomach, and to add dietary fiber to meals (see Prebiotics).
Prebiotics
Adding dietary fiber (or prebiotics) to your diet is recommended to boost the effectiveness of probiotics. According to Dr. Dash, prebiotics are “carbohydrates that selectively feed beneficial bacteria in the intestinal tract and stimulate their growth.” He explains that prebiotics may be thought of as “fertilizer” for the friendly bacteria in the microbiome.
Prebiotic supplements include polydextrose, inulin, beta-glucans, and fructooligosaccharides (FOS, also sometimes called oligofructose or oligofructan). Prebiotic foods include:
- Whole grains
- Fruits
- Vegetables
- Red wine
- Dark chocolate
Some of these foods also contribute to a fiber-rich diet, which helps relieve constipation—yet another benefit of probiotic use. Although it’s best to get fiber from whole foods, fiber supplements can be valuable, particularly if they include soluble fiber sources and are taken with lots of water.
Conclusion
Probiotics play an integral part in many of the body’s functions, including:
- Microbiome health
- Proper digestion
- Hormone balance
- Strengthening the immune system
- Prevention of allergy development
When trying to incorporate dietary or supplemental probiotics into your lifestyle, recommendations from your healthcare practitioner may help guide you to reliable products from proven manufacturers. Finding the right probiotic for your specific needs may help optimize microbiome health–and, by extension, overall wellness.
Connections is a publication of Women’s International Pharmacy, which is dedicated to the education and management of PMS, menopause, infertility, postpartum depression, and other hormone-related conditions and therapies.
This publication is distributed with the understanding that it does not constitute medical advice for individual problems. Although this material is intended to be accurate, proper medical advice should be sought from a competent healthcare professional.
Publisher: Constance Kindschi Hegerfeld, Executive VP – Women’s International Pharmacy
Authors: Carol Petersen, RPh, CNP; Reviewed and updated by Michelle Violi, PharmD – Women’s International Pharmacy
Co-Editors: Tami Haas; Laura Strommen – Women’s International Pharmacy
Illustrator: Amelia Janes – Midwest Educational Graphics
Copyright © Women’s International Pharmacy. This newsletter may be printed and photocopied for educational purposes, provided that your copy (or copies) include full copyright and contact information.
 For more information, please visit womensinternational.com or call 800.279.5708.
For more information, please visit womensinternational.com or call 800.279.5708.
Women’s International Pharmacy | Madison, WI 53718 | Youngtown, AZ 85363

