
Prostate Problems
Is Testosterone Really the Culprit?
For both men and women, testosterone is a vital hormone that performs many functions.
For men, the “prime of life” coincides with a time when testosterone levels are at their peak. Yet testosterone does not work alone. It combines with a plentiful enzyme called aromatase to produce small amounts of the estrogens, when and where they are needed.
Testosterone and the estrogens complement each other, working to keep each other’s power in check while serving many important health roles. In fact, male sexuality depends upon estrogens— as well as testosterone—because estrogens are essential to the brain chemistry that triggers a natural sexual function.
As men age, the ratio of testosterone to the estrogen hormones slowly changes. Between the ages of 25 and 50, a man’s testosterone level decreases by approximately 50%, while his estrogen levels increase by 50%. In addition, older men produce larger quantities of aromatase, causing them to convert more of their testosterone to estrogens, which then begin to “turn off” functions triggered by testosterone, such as building muscles and growing hair. This hormone shift, known as “andropause,” is a gradual one that can have devastating effects on male strength, energy, and sexual enjoyment. It also coincides with the onset of prostate problems.
For many years, it was thought that any increase in testosterone levels contributed to prostate cancer risk. This spurred controversy over the use of testosterone therapy. However, a recent review of the relevant medical literature, published in The New England Journal of Medicine, concluded that testosterone therapy is not associated with increases in the rate of prostate cancer or any other prostate illness.
 What Is the Prostate?
What Is the Prostate?
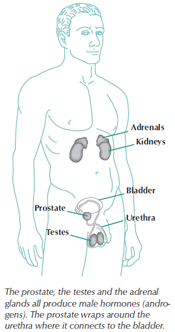
A healthy prostate gland is about the size of a walnut (see figure). It is located just below the bladder and above the rectum, and it surrounds the urethra. Its main role is to produce a thick liquid that makes up a substantial portion of a man’s semen. Muscles in the prostate help move sperm through the ejaculatory duct and also help open the bladder to allow urine to pass through the urethra. Thus, a healthy prostate gland is required for the satisfactory performance of both sexual and urinary functions.
We don’t know exactly how testosterone and the estrogen hormones work to maintain prostate health, but we do know that their role is undeniable. The prostate gland is highly unusual in that it increases in size four different times in a man’s life—at birth, puberty, young adulthood, and around age 50. It is probably not a coincidence that these growth spurts coincide with major hormonal changes.
Prostate Problems
When hearing “prostate problem,” men often think first of prostate cancer. Fortunately, prostate cancer tends to be very slow-growing and, when diagnosed early, is one of the most curable cancers. For this reason, most physical exams for men age 50 and over now include a thorough digital rectal exam to check the prostate. If there is any concern about potential prostate problems, the patient or healthcare practitioner may also request a blood draw for a PSA test, which measures a prostate-specific antigen (see box below). The healthcare practitioner is likely to consider the individual’s symptoms and family medical history, in addition to the exam and PSA test results, when evaluating prostate health.
The three primary health conditions that affect the prostate gland are prostatitis, enlarged prostate (benign prostatic hyperplasia, often shortened to BPH), and prostate cancer.
Prostatitis
Prostatitis, or inflammation of the prostate, is the least common prostate condition. It is most often found in men younger than 45 and is characterized by pain and discomfort in the pelvic area, irregular urination, and in acute cases, chills and fever.
“The prostate receives a plentiful blood supply, and periodically becomes congested—two of the characteristics of organs that are vulnerable to infections, both acute and chronic,” explains Aaron E. Katz, MD, founder of the Center for Holistic Urology at Columbia University Medical Center.
About 10% of prostatitis cases are bacterial and easily treated with antibiotics, with the remainder being a chronic, nonbacterial form whose origins are not well understood. In his 2006 Guide to Prostate Health, Dr. Katz notes that holistic medicine is an important part of the treatment for chronic prostatitis, which often does not respond to conventional therapies. His recommendations include lifestyle changes, hydrotherapy, and herbal and nutritional remedies.
Enlarged Prostate
By far the most common prostate illness is “enlarged prostate,” or benign prostatic hyperplasia (BPH), which is the abnormal but non-cancerous growth of prostate cells. Half of all men in the United States over age 60, and most men over the age of 70, will experience one or more of the following symptoms of an enlarged prostate:
- Increased frequency of urination
- Difficulty initiating urination
- Decreased force of urination
- Reduced urinary flow
- Urinary leakage
- Bladder fullness even after urination
- Painful urination
- Need to get up to urinate at night
- Extreme need to urinate
- Urinary blockage (a medical emergency)
As the prostate grows larger, it pushes against the urethra and bladder, blocking the normal urinary flow. Because the urethra—the tube that carries urine from the bladder to the penis—passes through the middle of the prostate gland, even a small amount of prostate enlargement can cause troublesome urinary symptoms.
It isn’t clear what causes the prostate gland to grow, but some theories involve a potent metabolite of testosterone called dihydrotestosterone (DHT). The prostate gland produces DHT by converting testosterone in the presence of an enzyme called 5-alpha reductase. As men age and their testosterone levels fall, DHT levels remain high, suggesting that this imbalance may be to blame. According to Dr. Katz, some studies suggest that men who do not produce DHT typically do not develop BPH.
Estrogens are also believed to play a role in the growth of both benign and cancerous prostate cells in aging men. In The Testosterone Syndrome, Dr. Eugene Shippen mentions a Japanese study in which men with the least prostate enlargement had higher testosterone levels, while those with the largest prostates had higher estrogen levels.
When BPH causes only mild symptoms, healthcare practitioners may advise “watchful waiting,” using frequent PSA tests and physical exams to monitor changes to the prostate. Practitioners may also recommend lifestyle changes, and/or herbal medicines and supplements. As symptoms start to worsen, Dr. Katz cautions that treatment should be considered because severe BPH can lead to serious health problems over time, including permanent bladder damage. Men who experience any symptoms of BPH—however minor—would be wise to see their healthcare practitioner to be evaluated for the most serious prostate condition: prostate cancer.
The PSA Test: What Does It Mean?
The PSA test is a blood test that checks for prostate-specific antigen (PSA), which is a protein produced by the prostate gland that may “leak” into the bloodstream. In Surviving Prostate Cancer Without Surgery, Dr. Bradley Hennenfent explains that “The more diseased your prostate, the more likely your prostate is to be swollen and to be leaking its PSA into your bloodstream and the more likely you are to be suffering from prostatitis, BPH or prostate cancer.” In general, the higher the PSA level, the more likely cancer is present. However, PSA levels must be interpreted individually and compared over time. While readings lower than 4.0 were previously thought to be normal, there is a growing consensus that an absolute cutoff level may not exist.
Since 1986, the PSA test has been credited with detecting more than 70% of all prostate cancers. Yet it is not a perfect gauge. A few men with prostate cancer have normal PSA levels. Conversely, most men with mildly or moderately elevated PSA levels do not have cancer; many have either BPH or prostatitis. Dr. Hennenfent cites studies showing that only 25 percent of men who had biopsies after a moderately elevated PSA test turned out to have prostate cancer. He argues that many biopsies could be avoided if practitioners simply treated BPH and prostatitis first.
Dr. Hennenfent believes that a single-minded focus on cancer detection negatively impacts men’s prostate health. “Why allow PSA levels as high as 4.0 to be considered normal, when anything over 1.0 probably indicates disease?” he writes. “Clearly doctors can step in much earlier to treat prostatitis and BPH, and possibly prevent prostate cancer.”
Prostate Cancer
According to the National Cancer Institute, prostate cancer is the second leading cause of cancer death among U.S. men, with nearly 31,000 men succumbing to this disease each year. It is believed to affect as many as 40 percent of men over age 50, and the incidence rises with age. Most patients are older, with 72 being the median age of diagnosis. If a man has a family history of prostate cancer, this is an increased risk, particularly if the relative was diagnosed prior to age 50. African Americans are also at higher risk for this cancer.
In its early stages and as the disease progresses, prostate cancer symptoms usually mirror those of BPH. Typically, the diagnosis is made when suspicious tissue is discovered during a digital rectal exam, prompting the healthcare practitioner to order a PSA test. When these results indicate the likelihood of cancer, a biopsy is performed.
While the cause of prostate cancer remains unknown, hormonal changes are strongly implicated. Lowering testosterone levels and/or manipulating its metabolism have proven to be important tools for treating existing prostate cancer. Thus, treatments for prostate cancer include a range of hormone therapies, often referred to as “androgen blockade.”
As its name implies, androgen blockade is designed to block one or more of the androgens (male hormones). The three organs shown in the figure produce these hormones. The testicles produce testosterone— by far the most plentiful male hormone. The adrenal glands secrete a small amount of several hormones known collectively as the “adrenal androgens” and the prostate produces DHT.
Other treatments for prostate cancer include surgery to remove the prostate, radiation, and chemotherapy. The options offered to any patient will vary depending on individual factors, such as their overall health and the aggressiveness of the cancer. Prostate cancer is typically very slow-growing (although this is not always the case). For older men with less aggressive tumors and men who are already in poor health, healthcare practitioners may simply advise “watchful waiting.”
Holistic practitioners often incorporate nutritional interventions to help thwart cancer. For example, Dr. Katz recommends that prostate cancer patients change their diets to reduce two factors that may feed prostate cancer: oxidation and inflammation. According to Katz, cancerous prostate tissue has higher measurements of oxidation than noncancerous tissue. Eating foods rich in antioxidants, such as fruits and vegetables, can help combat oxidation.
Oxidative stress goes hand in hand with inflammation, says Dr. Katz. He states that “some of the best minds in urological research are making a compelling case that chronic inflammation is a precursor of prostate cancer.” Dr. Katz recommends using anti-inflammatory herbs or supplements as a precautionary measure. Such herbs include holy basil, ginger, tumeric, green tea, oregano, rosemary, and several traditional Chinese herbs.
Testosterone Therapy and Prostate Cancer Risk
Numerous studies have established that severely limiting testosterone can cause prostate cancer to shrink, at least temporarily. From this fact grew the corresponding belief that raising testosterone levels would promote the growth of prostate cancer. A review of the medical literature performed by Dr. Ernani L. Rhoden and Dr. Abraham Morgentaler (published in the January 2004 issue of The New England Journal of Medicine) found no evidence that testosterone treatment causes prostate cancer, or that men with higher testosterone levels have higher rates of prostate cancer. In fact, they note that prostate cancer becomes more prevalent exactly at the time in a man’s life when testosterone levels decline. Testosterone therapy also did not consistently worsen the urinary symptoms experienced by men with prostate enlargement, say the authors. “The impact of testosterone therapy on benign prostate growth appears to be mild,” writes Dr. Rhoden, “and rarely of clinical significance.”
Another study in 2002 indicates that testosterone therapy may even benefit prostate health. The authors say 187 of 207 men with low testosterone levels who received testosterone therapy realized improvement in every parameter measured: their prostate glands all decreased in size, their PSA numbers went lower, and urinary symptoms such as frequency and urgency all improved.
Hormone Metabolism
When seeking to understand the effects of testosterone levels on the prostate gland, it is important to understand how the body metabolizes (breaks down) hormones. The key organ in this metabolism is the liver, which acts as a hormone processor. When the liver is unable to process hormones as quickly or effectively as it should, a hormone imbalance can result.
Estrogens, in particular, are slowly metabolized by the liver. For this reason, it is thought that improving estrogen metabolism may help improve hormone balance in older men.
Cruciferous vegetables, such as broccoli and cabbage, have been identified as helpful in maintaining balanced estrogen metabolites. When your body digests these vegetables, it produces a phytochemical called Indole-3-carbinol (I3C). Some studies show that it can inhibit the growth of prostate cancer cells.
Food supplements can have both positive and negative effects on estrogen metabolism, notes Dr. Shippen, who explains that grapefruit tends to inhibit the liver’s breakdown of estrogens, while cruciferous vegetables, such as broccoli and cauliflower, stimulate it. Zinc is believed to be especially helpful because it inhibits aromatase, the enzyme used by testosterone to create estrogens. “Many men will restore a proper balance of testosterone to estrogen purely through the use of zinc,” says Dr. Shippen.
A vicious cycle can begin for a middle-aged man struggling to achieve and maintain hormone balance, Dr. Shippen explains. A declining testosterone level “predisposes him to weight gain. Weight gain increases his estrogen level and estrogen stimulates SHBG [sex hormone-binding globulin, a protein in the blood that binds testosterone] … crippling the effectiveness of the hormone, which may cause more weight gain, which increases estrogen and so on.”
In addition, alcohol use can lower the liver’s ability to properly eliminate estrogens from the body, Dr. Shippen adds, while age and zinc deficiencies may increase aromatase, causing more of a man’s testosterone to be turned into estrogens, further stimulating SHBG, which repeats the cycle.
Conclusion
All organs of the male reproductive system, including the prostate, tend to stay healthy in the presence of adequate levels of key hormones, including testosterone, says Dr. Shippen. “Normal concentrations of testosterone and its more powerful derivative may well be harbingers of prostatic health, not illness.”
Connections is a publication of Women’s International Pharmacy, which is dedicated to the education and management of PMS, menopause, infertility, postpartum depression, and other hormone-related conditions and therapies.
This publication is distributed with the understanding that it does not constitute medical advice for individual problems. Although this material is intended to be accurate, proper medical advice should be sought from a competent healthcare professional.
Publisher: Constance Kindschi Hegerfeld, Executive VP – Women’s International Pharmacy
Co-Editors: Julie Johnson; Carol Petersen, RPh, CNP – Women’s International Pharmacy
Writer: Kathleen McCormick – McCormick Communications
Illustrator: Amelia Janes – Midwest Educational Graphics
Copyright © Women’s International Pharmacy. This newsletter may be printed and photocopied for educational purposes, provided that your copy (or copies) include full copyright and contact information.
 For more information, please visit womensinternational.com or call 800.279.5708.
For more information, please visit womensinternational.com or call 800.279.5708.
Women’s International Pharmacy | Madison, WI 53718 | Youngtown, AZ 85363

